There is a brand new virus that has recently swept the planet called

covid-19. Contained within this article is information regarding this virus including: definition, prevention and precautions. This is COVID19: the facts.
What is COVID-19

COVID-19 is the name given to the disease related to the virus: Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2). This is a brand new strain of corona virus that has not been previously identified in humans.
Corona viruses are viruses that pass among animals with a number of them also known to infect humans.
Bats are believed to be natural hosts of corona viruses although several other species of animals also are known to be a source. For instance, the Middle East Respiratory Syndrome Coronavirus (MERS-CoV) is transmitted to individuals from camels, and also the Severe Acute Respiratory Syndrome Coronavirus-1 (SARS-CoV-1) is transmitted to individuals from civet cats. More information on corona viruses can be found on the ECDC fact sheet.
How does COVID-19 spread (How can you get it)
Although animals are the first origin of the virus, it’s now spreading from person to person (human-to-human ) transmission. There’s not enough  epidemiological data at this point to confirm how easily and sustainably this virus spreads between people, but it’s currently estimated that, on the average, one infected person will infect between two and three more. The virus seems to be transmitted primarily by respiratory droplets that individuals sneeze, cough, or exhale. The virus additionally can live for several hours on exterior surfaces like tables and door handles. [More on this to follow]
epidemiological data at this point to confirm how easily and sustainably this virus spreads between people, but it’s currently estimated that, on the average, one infected person will infect between two and three more. The virus seems to be transmitted primarily by respiratory droplets that individuals sneeze, cough, or exhale. The virus additionally can live for several hours on exterior surfaces like tables and door handles. [More on this to follow]
The time period for COVID-19 (i.e. the time between exposure to the virus and beginning of symptoms) is currently estimated at between two and 14 days. At this stage, we all know that the virus is often transmitted when people that are infected show flu-like symptoms like coughing. There’s verification indicative that transmission can occur from an infected person with no symptoms; however, uncertainties remain about the effect of transmission by non symptomatic persons on the epidemic.
What are the symptoms of COVID-19 infection
COVID-19 can cause mild, flu-like symptoms such as:

- Fever.
- Cough.
- Shortness of breath or difficulty breathing.
- Chills.
- Repeated shaking with chills.
- Muscle pain.
- Headache.
- Sore throat.
- New loss of taste or smell.
More serious cases will develop severe pneumonia, acute respiratory distress syndrome, sepsis and septic shock that may cause death.
Keep in mind that individuals can be asymptomatic with no symptoms. However, they can still infect others without even knowing it.
Preliminary findings indicate that the death rate for COVID-19 is 20-30 per thousand people diagnosed. This is often significantly less than the 2003 SARS outbreak. However, it’s much more than the death rate for seasonal influenza.
The difference between COVID-19 and allergy symptoms
With this being allergy season, one may be concerned when symptoms arise. Below is a list of items that don’t usually accompany allergies:
- Sneezing
- Fever
- Shortness of breath
- Difficulty speaking and walking
Who is at risk
In most cases, elderly people and individuals with underlying health conditions (e.g. hypertension, diabetes, cardiovascular disease, chronic respiratory illness and cancer) are considered to be more in danger of developing severe symptoms.
As for youngsters, the disease appears to be relatively rare and mild. A sizable study from China suggested that just over 2% of cases were under 18 years old. Out of these subjects, fewer than 3% developed critical or grave disease.
As for pregnant women, at the time of this writing there’s limited scientific evidence on how severe of an illness occurs in pregnant women after COVID-19 infection. Having said that, current evidence suggests that severity of illness among pregnant women after COVID-19 infection is comparable to non-pregnant adult COVID-19 cases, and there is no data to suggest that infection with COVID-19 during pregnancy has a negative effect on the fetus. At the present time, there’s no evidence of transmission of COVID-19 from mother to child occurring during pregnancy. The Eu Centre for Disease Prevention and Control (ECDC) will still observe the prevailing scientific literature on this question, and suggests that every pregnant woman follow the identical precautions for the prevention of COVID-19, including regular hand washing, avoiding individuals who are sick, and self-isolating in the case of any symptoms, while consulting their healthcare professional for advice by telephone.
How to prevent COVID-19 infection

The virus enters the body through the eyes, nose and/or mouth, therefore it’s crucial to avoid touching your face with unwashed hands.
The washing of hands with soap and water for a minimum of 20 seconds, or cleaning hands with alcohol-based solutions, gels or wipes is strongly recommended in all surroundings. Washing-sanitizing your hands and sterilizing surfaces can help diminish your risk for becoming infected with this and other viruses.
It is also recommended to remain 3 ½ meters ((Approx 10 ft.) or faraway as possible from people infected with COVID-19 who are showing symptoms, to scale back the danger of infection through respiratory droplets.
In fact, it’s better to practice an action that has taken place in some locations—social distancing.
Social distancing is purposely escalating the physical space between individuals to avoid spreading illness. Staying a minimum of six feet far away from other people lessen your chances of catching the disease.
More illustrations of social distancing that allow avoiding larger crowds or crowded spaces are:
- Visiting loved ones by electronic devices rather face to face
- Working from the home as an alternative of the office
- Canceling or postponing conferences and sizable meetings
- Closing schools or switching to online classes
Further it’s important to take note that the virus can survive on surfaces for various periods of time. Therefore, it may be possible to contact the virus by touching a contaminated surface and then touching the eyes, nose, or mouth. As of this writing, the virus lasts on the following surfaces:
- On copper surfaces 3hrs.
- On cardboard 24 hrs.
- On Plastic and Stainless Steel 2-3 days
- In the Air 3 hrs.
For further explanation you can select this link.
What is the treatment for COVID-19
There are currently no vaccines against human corona viruses, including the virus that causes COVID-19. This is the reason why it’s extremely important to forestall infection and to contain additional spread of the virus.
The development of vaccines takes time. Several pharmaceutical companies are currently performing trials on vaccine candidates. However, it’ll take months or years before any vaccine will be widely used, because it must undergo extensive testing to establish its safety and effectiveness.
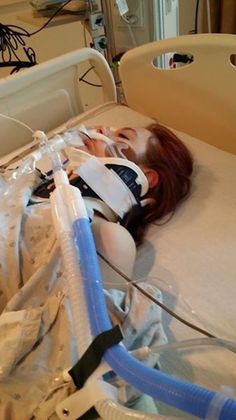
There is no specific treatment for this COVID-19, so healthcare providers treat the clinical symptoms (e.g. fever, difficulty breathing) of patients. Supportive care (e.g. fluid management, oxygen therapy etc.) can be very efficient for patients with symptoms.
Further, influenza and the virus that causes COVID-19 are two very different viruses and the seasonal influenza vaccine will not protect against COVID-19.
When to get tested for COVID-19
Current advice for testing depends on the stage of the outbreak in the country or area where one lives. Countries across the EU/EEA may be in different scenarios, even within the same country, and testing methods will be tailored to the situation at national and local levels.
National authorities may plan to only test subgroups of suspected cases supported by the national capacity to test, the supply of necessary equipment for testing, the extent of community transmission, or any other criteria. As a rational approach, national authorities may consider prioritizing testing in the following groups:
- elderly people with underlying chronic medical conditions such as lung disease, cancer, heart failure, renal disease, cerebrovascular disease (stroke victim), liver disease, diabetes, and immunocompromising conditions
- cases with critical respiratory infections in hospital or long-term care facilities;
- hospitalized patients with severe respiratory infections;
- patients with acute respiratory infections or influenza-like illness in certain outpatient clinics or hospitals in order to assess the extent of virus circulating in the population;
Where to get tested
If you’re feeling ill with COVID-19 symptoms (such as fever, cough, difficulty breathing, muscle pain or tiredness) it’s recommended that you contact your local healthcare services by telephone or online. If your healthcare provider believes there is a need for a laboratory test for the virus that causes COVID-19, he/she will inform you of the course of action to follow and advise you on where and how the test can be conducted.
What to do if you feel sick
Self-quarantine – Individuals who were exposed to the new corona virus and who are at risk for coming down with COVID-19 might practice self-quarantine. Healthcare professionals recommend that self-quarantine lasts 14 days. Two (2) weeks provide enough time for them to know whether they will become ill and be contagious to other people.
You might be asked to practice self-quarantine if you have recently returned from traveling to a part of the country or the world where the virus is spreading rapidly, or if you have knowingly been exposed to an infected person.
Self-quarantine involves:
- Staying at home
- Not having visitors
- Staying at least 6 feet away from other people in your household
- Using standard hygiene and washing hands frequently
- Not sharing things like towels and utensils
Once your quarantine period has ended, if you do not have symptoms, follow your doctor’s directions on how to return to your normal routine.
Isolation – For people that are confirmed to have the virus, isolation is required. Isolation is a health care term that indicates keeping people who are contaminated with a contagious illness away from those who are not contaminated. Isolation can occur at a residence or at a hospital or care facility. Special personal protective equipment must be used to attend to these patients in health care settings.
Should you wear a mask
Certain models of professional, tight-fitting respirators (e.g. the N95) can protect health care workers as they take care of infected patients.

Originally, face masks was not recommended for individuals. However the CDC (center for disease control) now know from recent studies that a significant portion of individuals with coronavirus lack symptoms (“asymptomatic”) and that even those who eventually develop symptoms (“pre-symptomatic”) can transmit the virus to others before showing symptoms. This means that the virus can spread between individuals mingling together in close distances to one another—for example, speaking, coughing, or sneezing, even if those people are not showing symptoms. In light of these new findings, CDC recommends wearing cloth face coverings in public settings where other social distancing measures are difficult to maintain (e.g., grocery stores and pharmacies) particularily in areas of substantial community based transmission.
- – Prevention tips
- Wash your hands often for at least 20 seconds at a time with warm water and soap.
- Don’t touch your face, eyes, nose, or mouth before you wash your hands.
- Don’t go about if you’re feeling ill or have any cold or flu symptoms.
- Stay at least 10 feet away from anyone who is coughing or sneezing and in general (social distancing).
- Cover your mouth with the inside of your elbow or tissue whenever you sneeze or cough. Throw away any tissues you use right away.
- Clean any objects you touch often. Use disinfectants on objects like phones, computers, utensils, dishware, and doorknobs.
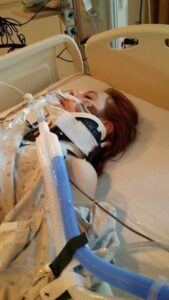
This disease can result in acute respiratory distress and must be taken very seriously. Prevention is better than cure and I urge the viewing of the video contained in this article that substantiates this fact.
Any question, comment or concern is welcomed below.
Good Health!!
At the moment the issue of covid-9 is very present everywhere and in some way it is affecting our lives. There is a lot of misinformation on the net and it is very gratifying to find this type of advice and guides because thanks to this you can take the necessary measures, definitely wearing a face mask like the one mentioned is highly recommended.
Actually, it is recommend that we don’t wear masks.
Thanks for stopping by and commenting!
COVID-19 epidemic has been a world scare as it treated even the greatest of the economy….thanks for this awesome and well-detailed article on covid-19 as I have seen anyone as detailed as this one……I learnt a lot from this article and I would share it to others so they can have a proper understanding of what they are dealing with…..
Thanks David – I’m so glad it helped. Thanks for commenting.