I recently wrote an article on the urinary system. In that article I mentioned the kidneys as one of the organs involved in that system. This article focuses exclusively on the kidneys and entails specific information and facts about the kidneys.
What are the kidneys
The kidneys are organs of the renal system. They are two (2) bean-shaped organs that play a major role in this system. They are located on either side of your spine, below the ribs and behind the abdomen. Each kidney is about four to five inches long, which is roughly the dimensions of a hefty fist.
What Do the Kidneys Do
The kidneys assist the body pass waste as urine. They also help filter blood before returning it back to the heart. The kidneys perform many critical 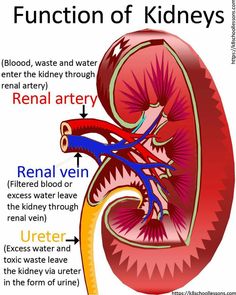 functions, including: regulating and filtering minerals from blood, maintaining overall fluid balance, generate hormones that help produce red blood cells, filtering waste materials from food, medications, and toxic substances, promote bone health, and regulate blood pressure. All of the blood of the body passes through them a number of times a day.
functions, including: regulating and filtering minerals from blood, maintaining overall fluid balance, generate hormones that help produce red blood cells, filtering waste materials from food, medications, and toxic substances, promote bone health, and regulate blood pressure. All of the blood of the body passes through them a number of times a day.
How Do the Kidneys Function
Blood flows into the kidney, waste gets removed, and salt, water, and minerals are adjusted, if needed. This filtered blood returns back into the body. The waste gets turned into urine that collects in the kidney’s pelvis which is a funnel-shaped structure that drains down a tube called the ureter a tube of muscle that pushes urine into the bladder.
Each kidney has around a million (1,000,000) tiny filters called nephrons. Nephrons are the most important part of the kidneys. They absorb blood, metabolize nutrients, and help pass out waste products from filtered blood. Each kidney has about 1 million nephrons and each has its own internal set of structures.
After blood enters a nephron, it goes into the Malpighian body, also called a renal corpuscle. The renal corpuscle contains two additional structures:
- The glomerulus. This is a collection of capillaries that take in protein from blood traveling through the renal corpuscle.
- The Bowman capsule. The residual fluid, called capsular urine, proceeds through the Bowman capsule into the renal tubules.
The renal tubules are a sequence of tubes that begin after the Bowman capsule and end at collecting ducts.
Each tubule has several parts:
- Proximal convoluted tubule. This section takes up water, sodium, and glucose and places them back into the blood.
- Loop of Henle. This section further takes up potassium, chloride, and sodium and places them into the blood.
- Distal convoluted tubule. This section takes in more sodium into the blood and takes in potassium and acid.
By the time fluid reaches the tip of the tubule, it’s diluted and crammed with urea. Urea is byproduct of protein metabolism that is released in urine.
Disorders of the Kidneys
As you can see, the kidneys perform a major in the overall function of the body. The body simply becomes overloaded with toxins if the kidneys can’t do their regular job. Because of all of the crucial functions the kidneys execute and the toxins they meet, the kidneys are subject to various problems.
Some of these conditions are:
Chronic renal disorder – is the progressive and irreversible destruction of the kidneys.
The most common causes of chronic renal disorder are high blood pressure and diabetes.
As mentioned earlier each kidney contains about 1 million tiny filtering units, called nephrons. Any disease that injures or scars the nephrons is capable of causing kidney disease. Both diabetes and high blood pressure (hypertension) can damage the nephrons.
High blood pressure can also damage the blood vessels of the kidneys, heart, and brain. The kidneys are highly vascularized, meaning they contain a lot of blood vessels. So, blood vessel diseases in general are dangerous to the kidneys.
Autoimmune diseases such as lupus can damage blood vessels and can make antibodies against kidney tissue.
There are various other causes of CKD. For example, renal disorder may be an explanation of CKD. Glomerulonephritis can be due to lupus. It can also appear after a streptococcal infection.
The risk of CKD increases for individuals older than age 65. The condition is also hereditary. It is more likely to occur in African-Americans, Native Americans, and Asian-Americans. Other risk factors for CKD include:
- obesity
- cigarette smoking
- high cholesterol
- kidney stones
- diabetes (types 1 and 2)
- atherosclerosis
- cirrhosis and liver failure
- narrowing of the artery that supplies your kidney
- obstructive kidney disease, including bladder obstruction caused by benign prostatic autoimmune disease
- hyperplasia
- kidney cancer
- bladder cancer
- kidney infection
- systemic lupus erythematosus
- scleroderma
- vasculitis
- vesicoureteral reflux, which occurs when urine flows back into the kidney
Kidney stones – Also known as renal calculi, are solid masses made of crystals. They usually originate in the kidneys. However, they can develop anywhere along the urinary tract, which consists of:
- kidneys

- ureters
- bladder
- urethra
Kidney stones are one of the most painful of medical conditions. The causes of kidney stones differ according to the type of stone. Not all kidney stones are made up of the identical crystals. The different types of kidney stones include:
Calcium – These are the most common. They are often made from calcium oxalate (though they will contain calcium phosphate or maleate). Eating fewer oxalate-rich foods can reduce the risk of developing this type of stone. High-oxalate foods include:
- spinach
- peanuts
- chocolate
- beets
- potato chips
However it is important to note that, even though some kidney stones are made of calcium, getting enough calcium in your diet can prevent stones from forming.
Uric acid – This type of kidney stone is more widespread in men than in women. They can arise in people with gout or those going through chemotherapy.
This form of stone develops when urine is just too acidic. A diet heavy in purines can raise urine’s acidic level. Purine a colorless substance found in animal proteins, like fish, shellfish, and meats is the culprit.
Struvite – This particular type of stone is found mostly in women with urinary tract infections (UTIs). These stones are often large and cause urinary obstruction. They are a consequence from a kidney infection. The treating of an underlying infection can prevent the progression of struvite stones.
Cystine – Cystine stones are rare. They occur in both males and females who have the genetic disease cystinuria. With this type of stone, cystine — an amino acid that materializes naturally in the body, leaks from the kidneys into the urine instead of remaining in the bloodstream.
The greatest risk factor for kidney stones is making under 1 liter of urine per day. Kidney stones are most presumably to occur in people between the ages of 20 and 50.
Different factors can increase the risk of developing a stone. In the US, Caucasian people are more likely to be inflicted with kidney stones than African American people.
Sex additionally plays a role. More men than women develop kidney stones, consistent with the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
A history of kidney stones can increase the risk. So does a family history of kidney stones.
Other risk factors include:
- dehydration
- hyperparathyroid condition
- obesity
- gastric bypass surgery
- a steady diet with excessive levels of protein, salt, or glucose
- inflammatory bowel diseases that increase calcium absorption
- consuming medications like triamterene diuretics, antiseizure drugs, and calcium-based antacids
Symptoms of kidney stones may not occur until the stone begins to maneuver down the ureters. Kidney stones are known to cause severe pain. This severe pain is called renal colic. There may be pain on one side of the back or abdomen. In men, the pain may expand to the groin area. The pain of this condition comes and goes, but is intense. Individuals with renal colic tend to be restless.
Other symptoms of kidney stones can include:
- vomiting
- nausea
- discolored or foul-smelling urine
- blood in the urine (red, pink, or brown urine)
- fever
- chills
- urinating small amounts of urine
- frequent need to urinate
Other kidney conditions include:
- kidney failure
- glomerulonephritis
- acute nephritis
- polycystic kidney disease
- urinary tract infections
- caliectasis
- acidosis
- uremia
- hydronephrosis
- pyelonephritis
- kidney cysts
- nephrotic syndrome
- azotemia
Symptoms of a Kidney Disorder
Kidney disorders can cause a range of symptoms. Some general ones include:
- back pain
- vomiting

- trouble sleeping
- fatigue
- inability to concentrate
- increased or decreased urination
- dry, itchy skin
- blood in urine
- constant foamy urine
- foot or ankle swelling
- puffiness around the eyes
- reduced appetite
- muscle cramps
An individual that experiences any of the above symptoms should contact their physician. Depending on the symptoms, he or she may do some kidney function tests to make a diagnosis.
Maintaining Healthy Kidneys
The kidneys are crucial organs and they affect many other body parts, including the heart. If we follow these tips it will help to keep them working efficiently:
Exercise – High blood pressure (Hypertension) is a known risk factor for chronic renal disorder. Regular exercise, even for just 20 minutes each day, can help reduce hypertension.

Stay hydrated – Drinking adequate amounts of water helps the kidneys
perform one of their most important functions: removing toxins. Learn more about what proportion of water you ought to be drinking a day.
Use medications with caution – Regularly taking certain over-the-counter medications like nonsteroidal anti-inflammatory drugs, can cause kidney damage over time. Occasionally taking them is all right, but work together with your doctor to seek out alternatives if you’ve got a condition that needs pain management, such as arthritis.
Other precautions:
- Eat less red meat – Red meat contains a hefty amount of iron, which can be really good for overall health, however, eating too much of it can damage the kidneys over time. This may be due to the fact that red meat produces too much dietary acid.
- Drink less soda – Soda contains copious amounts of sugar, artificial color, and sodium. It has very little nutritional value. Staying hydrated is crucial for kidney health, but it is better to get hydration from water rather than sugary sodas.
Drinking two or more sodas a day doubles the risk of kidney disease. Cola in addition contains phosphoric acid which has been confirmed to increase the risk of developing kidney disease. It is wise to limit soda intake to one can per week.
- Eat less shellfish – Fish and shellfish are a good source of protein, but, a 2014 study in the Journal of the American Society of Nephrology found that shellfish contain a toxic chemical called domoic acid. A condition:“Amnesic Shellfish Poisoning” can occur when too much shellfish is consumed, and this toxin can do irreparable harm to the kidneys. It’s the kidneys’ job to flush out toxins from your body, excessive amounts of this domoic acid passing through the kidneys, can simply overtax the system.
- Consume less salt – Eating too much salt can considerably increase the risk
 of developing kidney disease. Consuming excessive salt changes the level of sodium in the blood which can cause the kidneys to struggle to flush out excess water. It is wise to reduce salt intake, by eating fewer processed foods, cook at home more instead of eating out, and use herbs to add flavor to food to avoid relying too heavily on salt. Processed foods also contain high amounts of potassium and phosphorus.
of developing kidney disease. Consuming excessive salt changes the level of sodium in the blood which can cause the kidneys to struggle to flush out excess water. It is wise to reduce salt intake, by eating fewer processed foods, cook at home more instead of eating out, and use herbs to add flavor to food to avoid relying too heavily on salt. Processed foods also contain high amounts of potassium and phosphorus. - Limit energy drinks – Energy drinks contain lots of caffeine. Excess caffeine yields high blood pressure and stress, both of which lead to kidney damage. Another worry circles around the amino acid taurine. Frequently found in energy drinks and sports supplements, taurine tackles the kidneys head-on and is potentially dangerous to those with chronic kidney disorders.
- Beware of painkillers – Taking too many pain relievers can lead to a decrease in kidney function. According to a study in the New England Journal of Medicine, excessive use of pain relievers like Tylenol results in an outcome of 5,000 cases of kidney failure in the U.S. annually. These painkillers are most damaging to the kidneys when taken on an empty stomach. These painkillers should be consumed in moderation, and on a full stomach.
- Limit alcohol intake – Alcohol is a toxin that your body eventually needs to filter out. Drinking too much can put a real strain on the kidneys. The National Kidney Foundation defines over-drinking as “more than four drinks daily.” One drink equals a single glass, 12-ounce bottle, or shot. Not need to stop completely. Actually, a 2007 study found that people who drink in moderation actually reduce their risk of developing kidney disease by 30%.
- Don’t stop the flow – Holding urine is dangerous. It may sound strange but holding in urine is a primary cause of kidney problems. Urine contains bacteria, and the longer it stays in the body, the more bacteria it produces. It is very unhealthy for all of that bacterium to travel back up to the kidneys.
- Beware of butter – A recent health trend promotes replacing margarine with butter. In terms of the kidneys, this is not a good option. Butter contains saturated fats which, in high amounts, can damage the kidneys. According to the National Kidney Foundation, these fats raise LDL cholesterol (the “bad” kind) that harms the kidneys. It’s okay in small amounts. If margarine is used instead, it’s best that it be one with no Trans fat or “hydrogenated” fats. Trans fats are worse than saturated fats in raising LDL cholesterol.
- Watch the muscle building – Athletes who use steroids may gain muscle, but they’ll damage their kidneys. During a 2009 study, researchers found that nine out of ten bodybuilders resulted in kidney scarring from bodybuilding medications. When they ceased using these steroids, their kidneys healed over time. The American Society of Nephrology advises against steroids. They can elevate cholesterol levels, lower protein in the blood, and cause swelling–all of which harm the kidneys. While steroids can be used for some kidney treatments, it is not advisable to take bodybuilding medications recreationally.
There are more but bottom line: everything can have an effect on the kidneys because everything passes through them by way of the blood making them vulnerable to damage. Moderation is the key. Too much of anything can affect the kidneys. While there is so much in what we consume that is good for us, too much of a good thing is a bad thing.
Good balance is the key to life!
Any question comment or concern is welcomed below.
Good Health!!
 condition that is not typically diagnosed individually, but could affect the health of many people. In this article: what about leaky gut syndrome, light is shed on this condition.
condition that is not typically diagnosed individually, but could affect the health of many people. In this article: what about leaky gut syndrome, light is shed on this condition. to widen. When this occurs, the undigested food particles and toxins that are supposed to be blocked are allowed make their way into the bloodstream. Because these items are not normally allowed in the blood, they trigger the immune system to go into attack mode, which can often initiate allergies.
to widen. When this occurs, the undigested food particles and toxins that are supposed to be blocked are allowed make their way into the bloodstream. Because these items are not normally allowed in the blood, they trigger the immune system to go into attack mode, which can often initiate allergies.
 drink. It’s made using “starter” grains, just as sourdough bread has a “starter.” This starter is a combination of yeasts, milk proteins, and bacteria. It has a tart, creamy flavor, and it’s loaded with probiotic health benefits.
drink. It’s made using “starter” grains, just as sourdough bread has a “starter.” This starter is a combination of yeasts, milk proteins, and bacteria. It has a tart, creamy flavor, and it’s loaded with probiotic health benefits. by the medical experts because not all doctors agree that metabolic syndrome should be viewed as a distinct condition.
by the medical experts because not all doctors agree that metabolic syndrome should be viewed as a distinct condition.